

Anyone with acid reflux will tell you it’s very uncomfortable and they would love to rid themselves of it forever. While there’s no cure, specialists for acid reflux in Los Angeles can offer you treatments to soothe the issue. Contact a gastroesophageal reflux doctor in Los Angeles to set up an appointment to get your acid reflux under control.
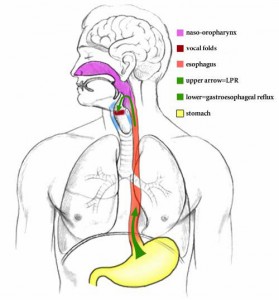
Gastroesophageal Reflux Disease (GERD) occurs when there is backward flow of stomach contents up into the esophagus. A related problem, addressed by ENT’s and gastroenterologists, is Laryngo Pharyngeal Reflux (LPR). Normally, the lower esophageal sphincter (LES), a ring-shaped muscle at the opening of the stomach, acts as a valve. This valve prevents backward flow of food and acid from the stomach. If the LES opens at the wrong time, the acidic contents of the stomach are allowed up into the esophagus, causing irritating symptoms and rarely more serious problems. The symptoms of LPR manifest when the acidic contents reach higher, into the back of the throat (Pharynx) and voice box (Larynx). This is a very common problem and is sometimes termed “silent reflux” due to lack of heartburn symptoms.
LPR can present with many symptoms. Typically it is one or a combination of the following recurrent symptoms:
These symptoms can occur at any age, including in children. Heartburn can also be present, although this is found in less than 50% of patients with LPR.
LA treatment of acid reflux consists of 3 stages:
This is by far the most important part of the treatment. Often, this alone helps relieve the symptoms of reflux. Try following the next steps as closely as possible (listed in order of importance).
This may imply a significant change in your lifestyle. However, once your symptoms have resolved (this may take up to 6 months) you may start reintroducing the things you liked (e.g. coffee, orange juice …) one at a time. If your symptoms recur, you’ll know that you need to stay away from those particular things.
Over-the-counter antacids, such as Maalox or Tums, provide marginal benefit, since they are only effective for a few hours. In cases not responding to lifestyle changes, a prescription medication may be recommended (such as Aciphex, Nexium, Prevacid, Prilosec, or Protonix). These may need to be taken once or twice a day, for an initial course of up to 6 months.
This option, though very effective, is rarely necessary and is reserved for the most severe, refractory cases. It involves physically narrowing the lower esophageal sphincter to minimize reflux of stomach contents. Your ENT doctor in Los Angeles will discuss these options with you if necessary.
Common Causes of Acid Reflux
As you read above, acid reflux is suffered by many people and has many causes. The first thing your head and neck doctor will suggest is treating acid reflux with lifestyle changes. The common causes of acid reflux are listed below:
For informational purposes only, a link to the federal Centers for Medicare and Medicaid Services (CMS) Open Payments web page is provided here at https://openpaymentsdata.cms.gov. The federal Physician Payments Sunshine Act requires that detailed information about payment and other payments of value worth over ten dollars ($10) from manufacturers of drugs, medical devices, and biologics to physicians and teaching hospitals be made available to the public.
*As of October 1st 2023, Dr. Shapiro will be an out of network provider. Dr. Shapiro’s services will be fee-for-service and are not contracted with any insurance company. Payments are to be paid in full at the time of each visit or prior to the date of surgery. The fee schedule is available upon request. As a courtesy to our patients and to maximize your reimbursement, the office will provide you with a claim form to be submitted to your insurance. For out of network care we do not verify insurance coverage and assume the insurance information you provide is accurate. Reimbursements will come directly to you from your insurance carrier based on your plan's out of network coverage and deductible. We do not bill secondary policies. Please note that all other fees (facility and anesthesia fees for surgery, and tests such as labs or x-rays) will still go through your insurance as per regular insurance in-network contract.
At Westside Head & Neck, it is our highest priority to protect the health of our patients, staff, and community. As an essential business dedicated to serving the community, we will remain open with modified hours. We have implemented all guidelines set by the CDC and Department of Health with regards to ensuring safety and additionally installed state-of-the-art viral filtration systems in all rooms. Click here to read more.
© Copyright 2013 - 2025 | West Side Head & Neck | All Rights Reserved.